Train derails in southeast Texas, forcing evacuations
October 29, 2020
Wall Street soared under Trump, but it's been a rocky ride
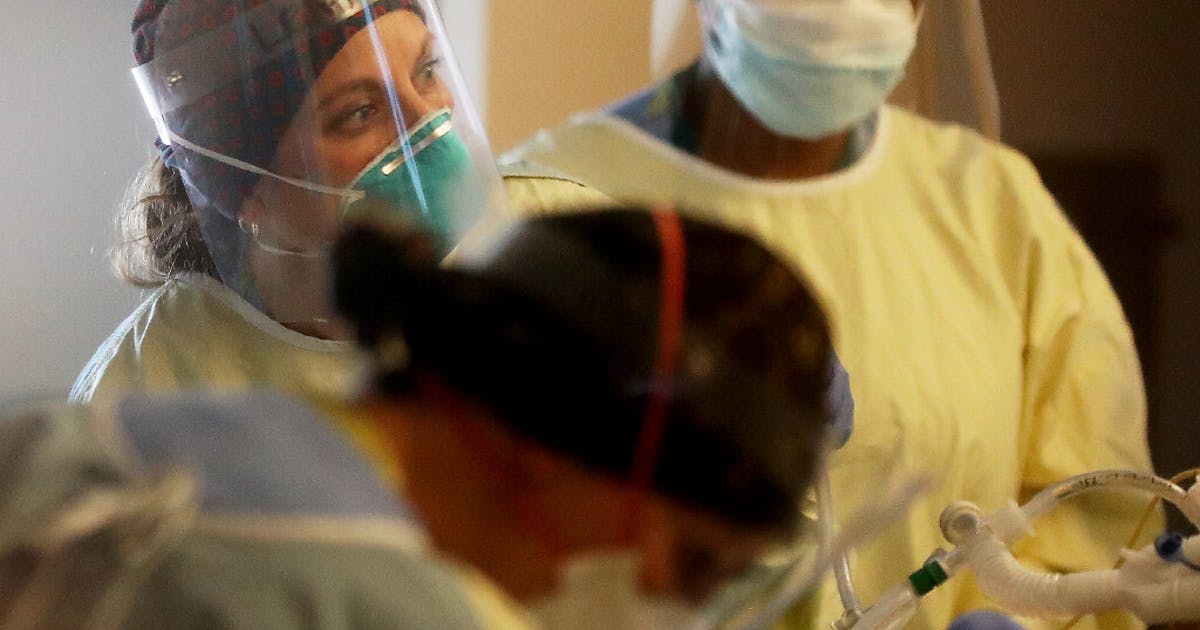
October 29, 2020Nurses and other bedside caregivers are far less likely to catch COVID-19 after risky exposures to patients, compared to interactions at home or in the community, new data show.
But caregivers are twice as likely to be diagnosed with COVID after risky exposures to a co-worker in the break rooms, as compared to patient exposures, according to an analysis of more than 5,000 higher-risk health care worker exposures between March and July in Minnesota, which was published Thursday.
Public health officials said Thursday that the data show the effectiveness of ubiquitous use of personal protective equipment in hospitals, including medical-grade face masks and eye protection.
Those same protections are not typically observed at home or in the community, which is a key reason for the higher risk of getting the virus from a community exposure. Interactions with contagious family members also tends to be more intimate and longer in duration, which increases risks.
But protective equipment only works when it’s available. The Minnesota Nurses Association said Thursday that workers are being exposed to COVID inside healthcare facilities as a direct result of the lack of proper protective equipment.
The nurses’ union also said exposures are driven by human resource policies at hospitals, including some that force workers to return to work before their quarantine period ends, and others that penalize nurses by withholding regular pay while they’re out of work for testing or quarantine.
The March-to-July data show that for higher-risk exposures to COVID-positive patients in the hospital, 1.3% are followed by positive diagnosis for COVID in the health care worker within 14 days, according to contact tracing.
In contrast, 3.8% of higher-risk exposures to COVID-positive co-workers on the job led to a positive case in the exposed worker.
And 12.5% of documented higher-risk exposures in the community or at home led to a positive diagnosis in the health care workers. Cases in which health care workers infect each other outside of work, like at a wedding, are included in the community-transmission statistic.
“That says to me that the personal protective equipment that has been chosen is working,” Sylvia Garcia-Houchins, director of infection prevention and control at the Joint Commission, said Thursday.
Labor officials said the study demonstrates the need for wider distribution of PPE at hospitals, among other things.
“We call on the [Minnesota Department of Health and Minnesota Hospital Association] to increase the supplies of PPE to all healthcare workers. No single percentage point, no single infection is acceptable when we can protect all healthcare workers,” the Minnesota Nurses Association said in a statement.
This is a developing story; check back for updates.