Volkswagen loses top court case in EU in diesel scandal
December 17, 2020
The Latest: France's Macron tests positive for COVID-19
December 17, 2020With Gov. Tim Walz using his emergency powers to close certain types of businesses and events, it’s important to get a handle on which types of businesses and events are linked to COVID-19 spread.
Unfortunately, our data here is somewhat limited. The state’s contact tracers interview people who test positive and ask them questions about their demographics and about the kind of activities they engaged in over the past two weeks. But the list isn’t exhaustive — we don’t have data, for example, on the share of people who went shopping before catching COVID-19. And contact tracers only manage to talk to a portion of all positive cases in the state — especially lately, as Minnesota’s November surge overwhelmed the state’s contact tracing capabilities.
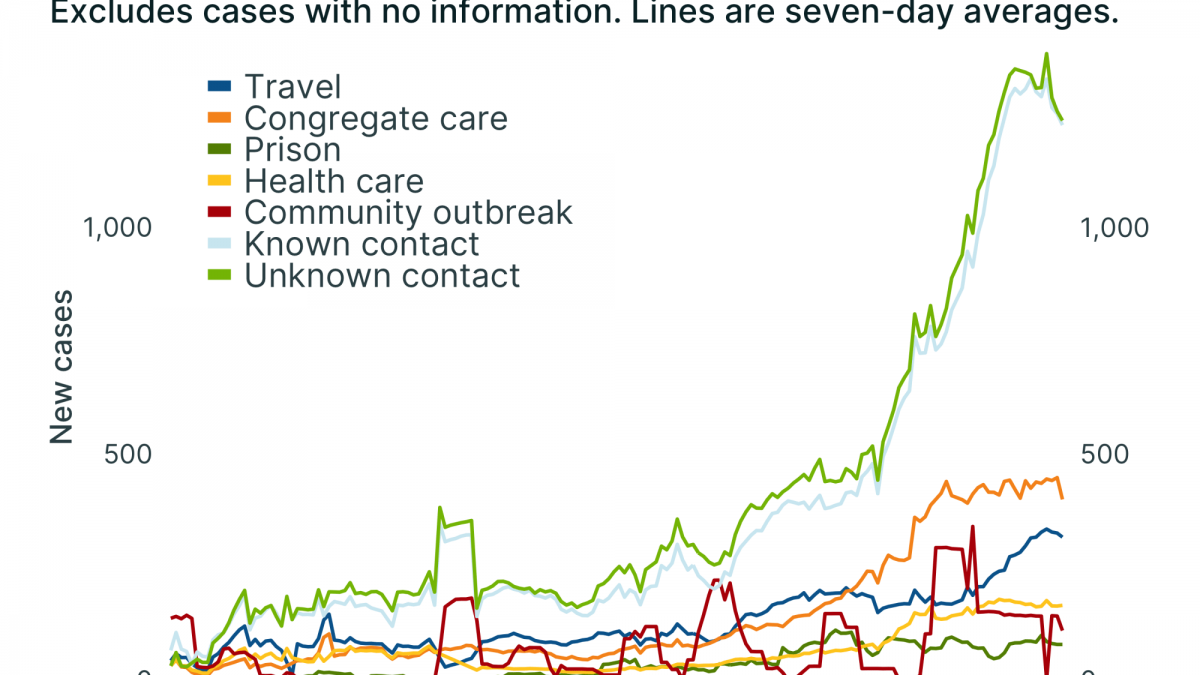
Here’s the overall likely exposure figures for those subset of cases who have spoken to contact tracers. You can see that the lion’s share of cases come from what’s called “community spread” — a catch-all for infections that aren’t linked to a specific setting or outbreak (such as a prison, nursing home, or an outbreak or a wedding). Of those about the same number were and weren’t able to tell contact tracers who they probably caught the disease from.
But as I said, significant numbers of Minnesota’s cases don’t speak to contact tracers. To put that in context, here’s that same chart, but with “unknown/missing” data added back in.
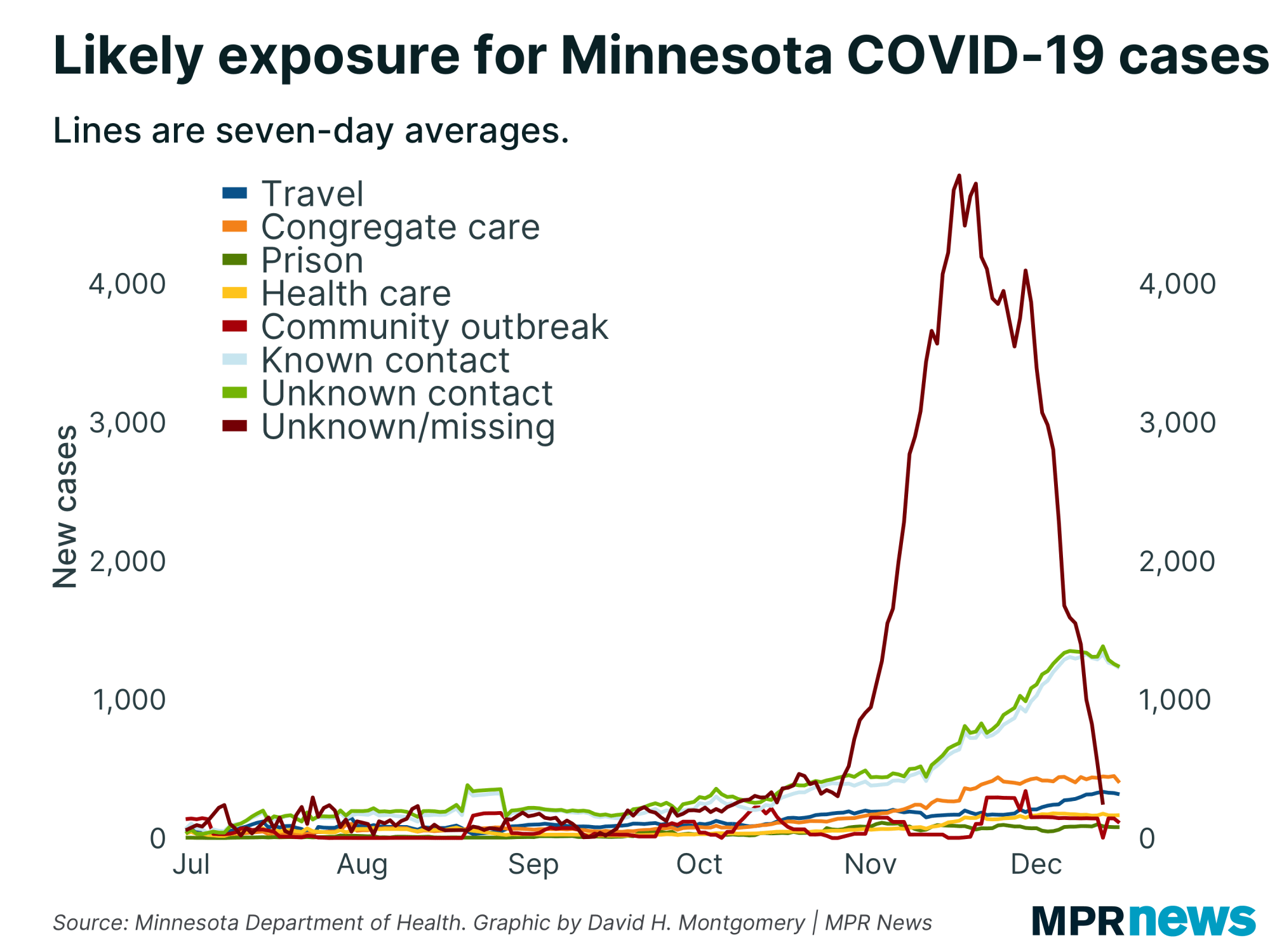
You see how it breaks the scale there.
Getting more specific, we have data on people who are linked to social settings, like restaurants, church, sporting events, weddings and parties. But here again, the data is murky.
For example, we have the number of cases linked to outbreaks at social settings. An “outbreak” is a technical term meaning a significant number of cases from different households tied to a single setting. (The exact number can vary, but for example, a restaurant outbreak is defined as “five [or more] unrelated cases from five households that mentioned only one restaurant/bar, within one month.”)
So if I go to a wedding, and get sick with COVID-19 a few days later, whether or not that wedding counts as an “outbreak” depends on whether a bunch of other, unrelated people at the same wedding also got sick.
As a share of overall cases, the number of cases linked to outbreaks at any one type of setting is pretty small. (Even all community outbreaks combined are pretty small — it’s the maroon line on the charts above.) For example, there were 7,087 confirmed cases linked to outbreaks at restaurants from June 10 to Dec. 10. That’s about 2 percent of all cases diagnosed during that time — a figure that the hospitality industry cites in its defense.
But that 2 percent figure isn’t the right math. Remember how many cases had unknown contact tracing data? The ideal math is not to divide the 7,087 cases linked to restaurant outbreaks by the 343,240 total cases over the timeframe — we don’t know anything at all about the exposure of the people who weren’t interviewed. It’s to divide 7,087 by the 186,397 cases with completed contact tracing over that time. That’s a somewhat higher 3.8 percent (and is, properly, stated as 3.8 percent of interviewed cases, not 3.8 percent of all cases).
Below, you can see major categories of social event and the share of interviewed cases linked to an outbreak there:

But that’s not the only way to look at this data. Remember that only a small share of all cases were linked to outbreaks at all, which is a pretty limited definition requiring lots of confirmed cases linked to a particular event. We can also look at data about how many sick people said they had attended any of these types of establishments during the 14 days before they got sick.
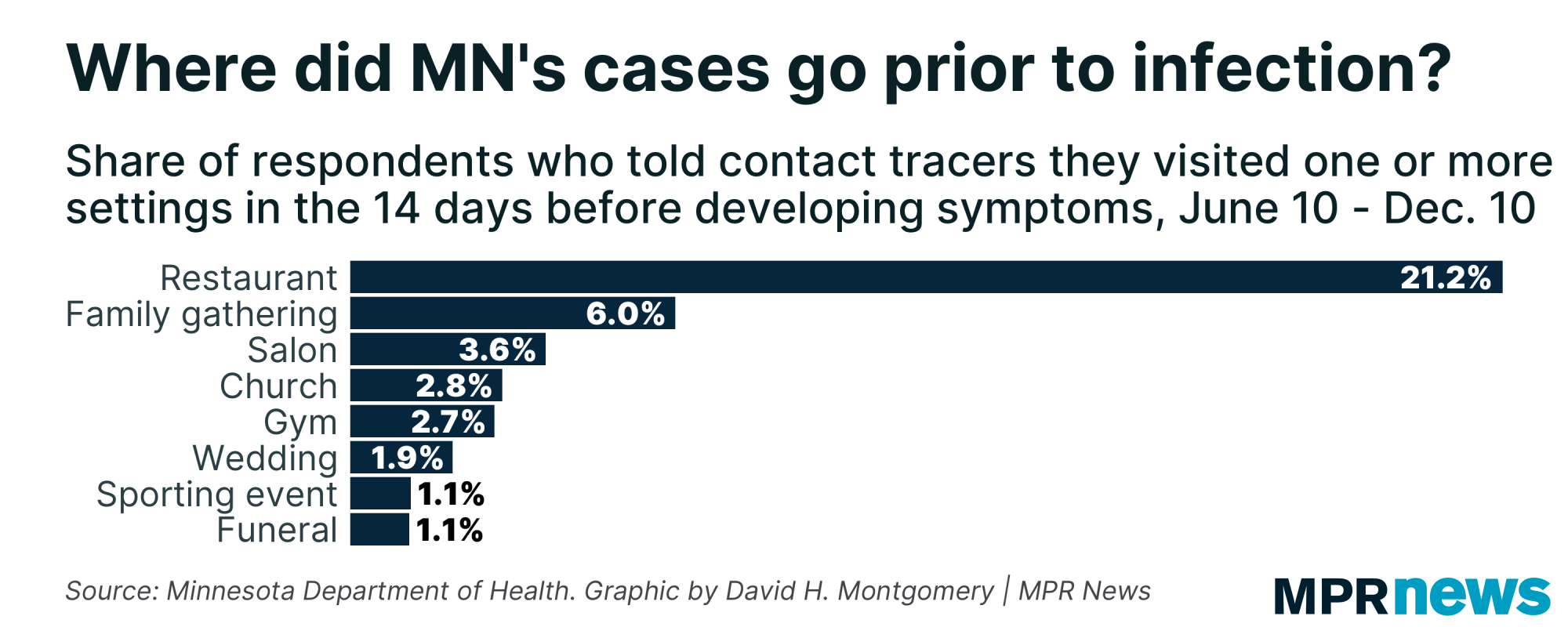
Here we get much larger numbers — more than 20 percent of interviewed people who got COVID-19 said they had eaten at a restaurant in the two weeks before getting sick, while 6 percent had been to a family gathering, and 3.6 percent had gone to a salon.
Again I’ll strongly caution you against over-interpreting this chart. This isn’t a chart of where people got sick — just where they went. And not all activities on here have the same risk factor for catching COVID-19 — if you asked people how many had gone for a walk in the past 14 days, the number might very well be higher than 21.2 percent, but that doesn’t mean going for walks is more dangerous than eating at restaurants. Just as the above chart of cases from confirmed outbreaks likely underestimates the share of interviewed people who got sick at a given type of event, this probably overestimates it. The point is, it’s a complicated question with inexact data that makes it impossible to speak with certainty. Anyone who says otherwise is trying to sell you something.
So what does this mean for judging Walz’s “pause” for inside service at restaurants? My job isn’t to tell you whether a given policy should or should not be implemented, but rather to give you information you can use to better make those decisions yourself.
It’s clearly the case that, with the limited data we have, restaurants appear to be linked to a lot more cases than other social activities. But this doesn’t let us compare the relative risk of events like eating at a restaurant versus having some friends over for dinner versus going Christmas shopping at a mall. (To do that, we’d need to be able to at the very least control for frequency: For every visit to a restaurant, how many people got sick? We just don’t have that data.)
You make MPR News possible. Individual donations are behind the clarity in coverage from our reporters across the state, stories that connect us, and conversations that provide perspectives. Help ensure MPR remains a resource that brings Minnesotans together.